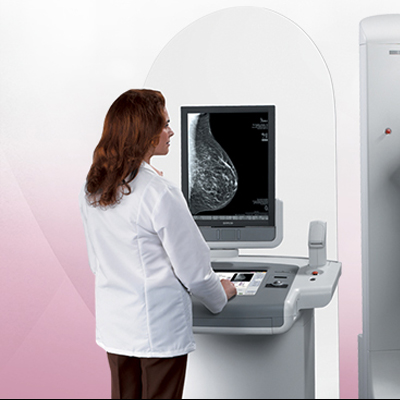
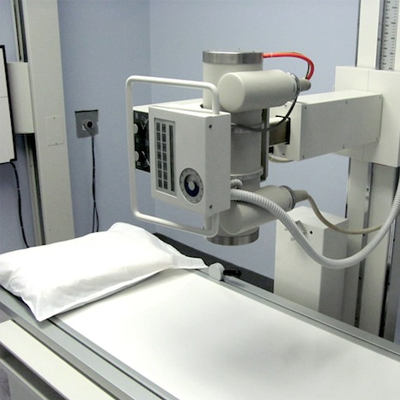
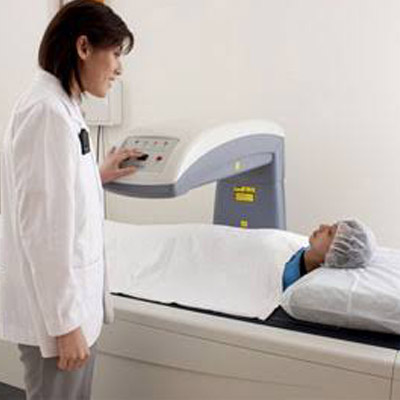
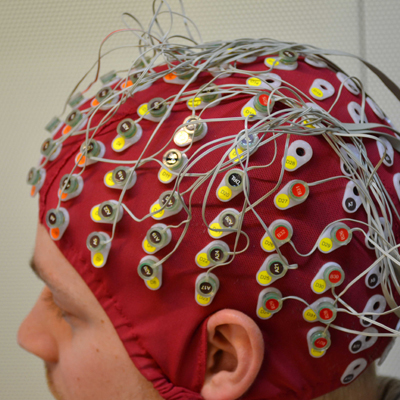
RADIOLOGY & Imaging tests
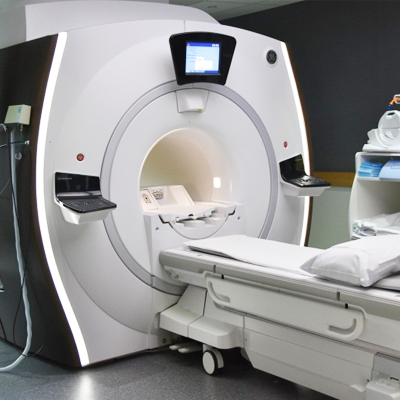
3 Tesla Silent MRI
VIEW DETAILS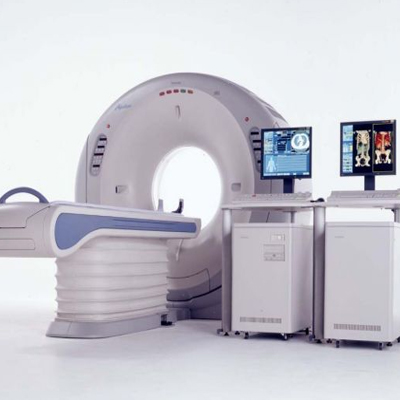
Multi-Slice CT Scan
VIEW DETAILS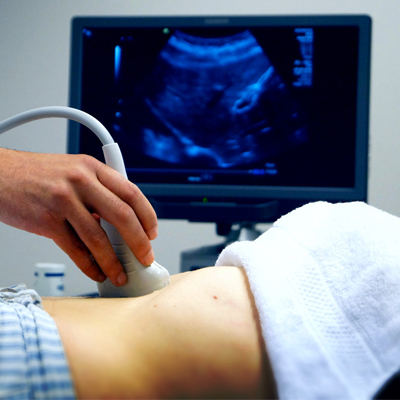
Ultrasound Imaging
VIEW DETAILS
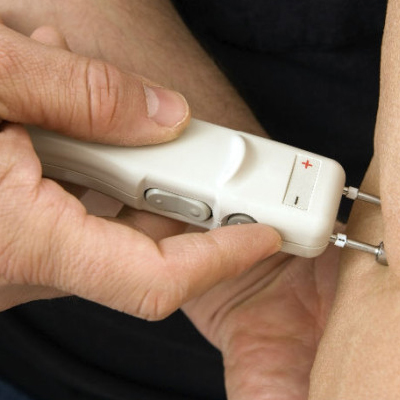
FibroScan
VIEW DETAILSCARDIOLOGY TESTS
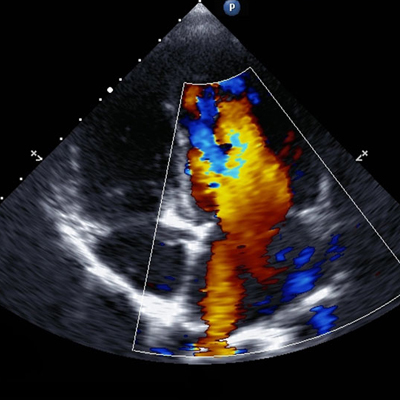
Echocardiogram
VIEW DETAILS
TMT/Stress Test
VIEW DETAILS
Holter
VIEW DETAILS
ECG
VIEW DETAILSPulmonary Function Test
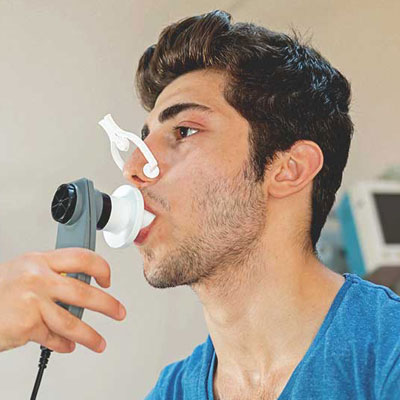
Pulmonary function test
VIEW DETAILSLABORATORY TESTS
GENNext Diagnostics offers a complete menu of clinical diagnostic tests. The fully automated lab has state-of-art fully automated blood analyzing instruments from reputed Global companies like Siemens, Roche, Becton Dickinson, Sysmex and Transaia. Quality in testing is achieved by systematic alignment of test reagents machinery and man behind the machinery. There are daily rigorous checks which ensure quality control and assurance of reagents and machinery. Standard Operation Procedures and checklists ensure that our highly experienced work force delivers accurate and precise results every time. All the samples received are bar-coded and collected by zero-contact' collection method in designated vaccutainer. All the equipments have direct interfacing of results from equipment to a customized high-end Laboratory Information Management System. All of this results in accuracy par excellence!
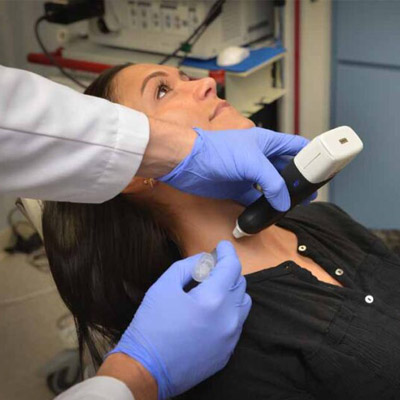
FNAC test
VIEW DETAILSDiagnostics Equipments at GENNext Diagnostics
- Real-time automated PCR
- Fully automated Immunoassay analyzer (Roche e411)
- Fully automated biochemistry analyzer
- Fully automated 6 part hematology analyzer (SYSMEX)
- Fully automated blood culture system (BD BACTEC)
- Fully automated Culture Identification and AST system (BD Phoenix)
- Fully automated ELISA processor (ERBA)
- Automated Coagulation Analyzer
- Automated Electrolytes Analyzer
- Automated Urine Analyzer
- Automated Semen Analyzer
Hospital Infection Control
The care of critically ill patients in the intensive care unit (ICU) is a basic feature of modern hospital setup. Nosocomial infections are one of the most common complications that occur in ICU patients. The incidence of nosocomial infection or hospital-acquired infections is about 5-10% in Indian setup. Hospital infection control programs can prevent approx. 33% of nosocomial infections. Diagnostic procedures, medical devices, medical and surgical treatment are risk factors in the hospital environment. The occurrence of these infections has consequences such as increased risk of mortality (double or triple), prolonged hospital stays, and increased medical expenses. Patients in the ICU are often receiving high doses of various antibiotics, are in close proximity to each other, and are being cared for by busy physicians and nurses. All these factors create an ideal environment for developing and transmitting resistant organisms. Specific types of antibiotic-resistant microorganisms vary with the type of unit, patient population, procedures, associated equipment, and antibiotic usage.
The ICU is an important reservoir of antibiotic-resistant bacteria that may spread to other clinical areas of the hospital. The widespread, empirical use of broad-spectrum antibiotics, while often clinically appropriate, selects resistant microbes for survival; these readily colonize critically ill patients. Poor compliance with hand-washing protocols (especially among the medical staff), nurse shortages, and the crowding of patients and their relatives promote horizontal transmission of resistant strains.
Detection, control and preventive measures are of the utmost importance in every ICU. These methods include microbiological surveillance of ICU/NICU/Operation theaters, isolating patients, washing hands, using protective clothing, cleaning and disinfecting equipment, cleaning the environment, and providing education and training. We believe that by monitoring hospital infections and then communicating results to the hospital administrators and consultants is very important to the quality of medical care delivered. By detecting abnormal factors in the environment and correcting them, hospitals can control infections in the ICU and thus can give better care to their patients. This also gives a ‘good name’ to the place and people who are associated with it.
We look forward to have an opportunity to offer our professional services to your establishment. Please enquire at 7051774777 for further details.